What Is Parenteral Nutrition
Overview of Parenteral Nutrition
Parenteral nutrition (PN) is intravenous administration of nutrition, which may include protein, carbohydrate, fat, minerals and electrolytes, vitamins and other trace elements for patients who cannot eat or absorb enough food through tube feeding formula or by mouth to maintain good nutrition status. Achieving the right nutritional intake in a timely manner can help combat complications and be an important part of a patient’s recovery. Parenteral nutrition is sometimes called Total Parenteral Nutrition (TPN).
Who Receives Parenteral Nutrition?
People of all ages receive parenteral nutrition. It may be given to infants and children, as well as to adults.
People can live well on parenteral nutrition for as long as it is needed. Many times, parenteral nutrition is used for a short time; then it is lessened or discontinued when the person begins to switch to tube feeding or eat enough by mouth. Parenteral nutrition bypasses the normal digestion in the gastrointestinal (GI) tract. It is a sterile liquid chemical formula given directly into the bloodstream through an intravenous (IV) catheter (needle in the vein).
For What Diseases or Conditions Would Patients Need PN?
Patients may need PN for any variety of diseases or conditions that impair food intake, nutrient digestion or absorption. Some diseases and conditions where PN is indicated include but are not limited to short bowel syndrome, GI fistulas, bowel obstruction, critically ill patients, and severe acute pancreatitis. Some patients may require this therapy for a short time and there are other patients who have received PN at home for a lifetime.
What are the side effects of parenteral nutrition?
The most common side effects of parenteral nutrition are mouth sores, poor night vision, and skin changes. You should speak with your doctor if these conditions don’t go away.
Other less common side effects include:
- changes in heartbeat
- confusion
- convulsions or seizures
- difficulty breathing
- fast weight gain or weight loss
- fatigue
- fever or chills
- increased urination
- jumpy reflexes
- memory loss
- muscle twitching, weakness, or cramps
- stomach pain
- swelling of your hands, feet, or legs
- thirst
- tingling in your hands or feet
- vomiting
How do you prepare for parenteral nutrition?
You need to speak with your healthcare provider about your exact nutritional needs. Your provider will prescribe the appropriate liquid for fulfilling these needs. You store this liquid in a refrigerator or freezer.
Each dose must be removed from the fridge four to six hours before use. This allows enough time for the liquid to reach room temperature. Frozen packets should be moved to the refrigerator 24 hours before use to thaw.
How is parenteral nutrition administered?
Parenteral nutrition is administered from a bag containing the nutrients you need through tubing attached to a needle or catheter.
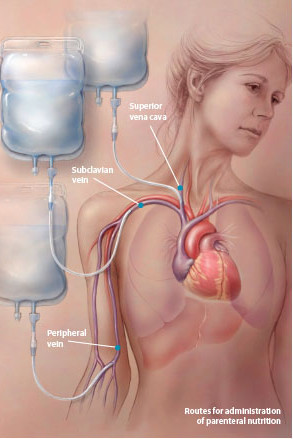
With TPN, your healthcare provider places the catheter in a large vein, called the superior vena cava, that goes to your heart. Your healthcare provider may also place a port, such as a needleless access port, which makes intravenous feeding easier.
For temporary nutritional needs, your doctor may suggest PPN. This type of intravenous feeding uses a regular peripheral intravenous line instead of a central line threaded into your superior vena cava.
You’ll most likely complete intravenous feedings yourself at home. It usually takes 10 to 12 hours, and you’ll repeat this procedure five to seven times a week.
Your healthcare provider will provide detailed instructions for this procedure. In general, you first need to check your nutrient bags for floating particles and discoloration. Then you insert tubing into the bag and attach the tubing to your intravenous catheter or port as designated by your healthcare provider.
You need to leave the bag and tubing in place for most or all of the day. Afterward, you remove the nutrient bag and tubing.
What are the risks of parenteral nutrition?
The most common risk of using parenteral nutrition is developing catheter infection. Other risks include:
- blood clots
- liver disease
- bone disease
It’s essential to maintain clean tubing, needleless access ports, catheters, and other equipment to minimize these risks.
What is the outlook after parenteral nutrition?
Many people experience some improvement in their condition after parenteral nutrition. You may not be rid of your symptoms, but your body may be able to heal more quickly. You’ll likely feel stronger and more energized. This can help you do more in spite of the effects of your condition.
A physician or dietitian will reassess your nutritional needs after several weeks of this nutrition program to see if any adjustments need to be made in the dosage. You’ll likely have tests done to assess your individual needs.
The results of parenteral nutrition are maintained health and energy levels in your body. You may need this treatment only temporarily. Or you may need to use it for the rest of your life. Your nutritional needs may change with time.
Resources:
http://www.nutritioncare.org/about_clinical_nutrition/what_is_parenteral_nutrition/
https://www.healthline.com/health/parenteral-nutrition#side-effects